Imagine being rushed to open-heart surgery because of irregular heart activity only to be immediately discharged because there were not any obvious signs of heart disease. This happened to heart health patient advocate Denise Johnson, who was sent straight to surgery after readings from a stress test showed a possible heart attack, only to be sent home without answers.

While enjoying a relaxing evening at home, Denise started feeling incredible pressure on her chest that radiated pain across her back and down her arm. “My heart was racing and when I took a blood pressure measurement the next morning at a local pharmacy, it was quite high,” shares Denise. “With both my friend and the pharmacist expressing concern about my high blood pressure, I went to emergency where I received a CT scan of my heart. No irregularities showed up so I was asked to see my family doctor. She recognized how unusual it was for me to have high blood pressure and booked me for a stress test a few weeks later. I felt great while running during the test, there was no discomfort, but I was immediately told to stop as those monitoring the test said it looked like I was having a heart attack. I was brought to urgent care where a cardiologist informed me that my stress test was very irregular and I should notify my next-of-kin as I may need open-heart surgery.”
After arriving at the hospital via ambulance, Denise was rushed to the operating room where a scope was used to view the large vessels inside her heart. “I was awake, watching the screen, because I wanted to see what was wrong with my heart. The surgeon came in, looked at the screen, and told the staff that I didn’t need heart surgery because I had hardly any plaque build-up inside my arteries and my heart muscle was strong. There was no obvious evidence of a heart attack.”
Solving a mystery

Classic heart attack symptoms, such as crushing central chest pain followed by light-headedness and collapsing, are widely recognized by both the public and the health care community. However, data supporting these symptoms were often collected from predominantly male patient populations, where heart attacks commonly present as blockages within the large arteries of the heart. As illustrated by Denise’s experience, this is not always the case.
“Fifty percent of heart attacks are missed in women who show up to the emergency department with chest pain concerns,” highlights Dr. Karin Humphries, CHÉOS’ Program Head of Cardiovascular Health. “Many women who have heart attacks describe their chest pain as pressure or squeezing and often have additional symptoms including nausea, discomfort in the back, neck, or jaw, and shortness of breath, which are not yet widely recognized as heart attack symptoms. They are told it’s anxiety, depression, or ‘all in your head’, which is often not the case.”
Women-focused care
Still concerned about her heart and the irregular stress test results, Denise worked closely with her family doctor to manage her health until they found an expert who understood women’s heart health. She was referred to Advancing Health Scientist and Director of the Leslie Diamond Women’s Heart Centre Dr. Tara Sedlak, who specializes in women’s heart health.

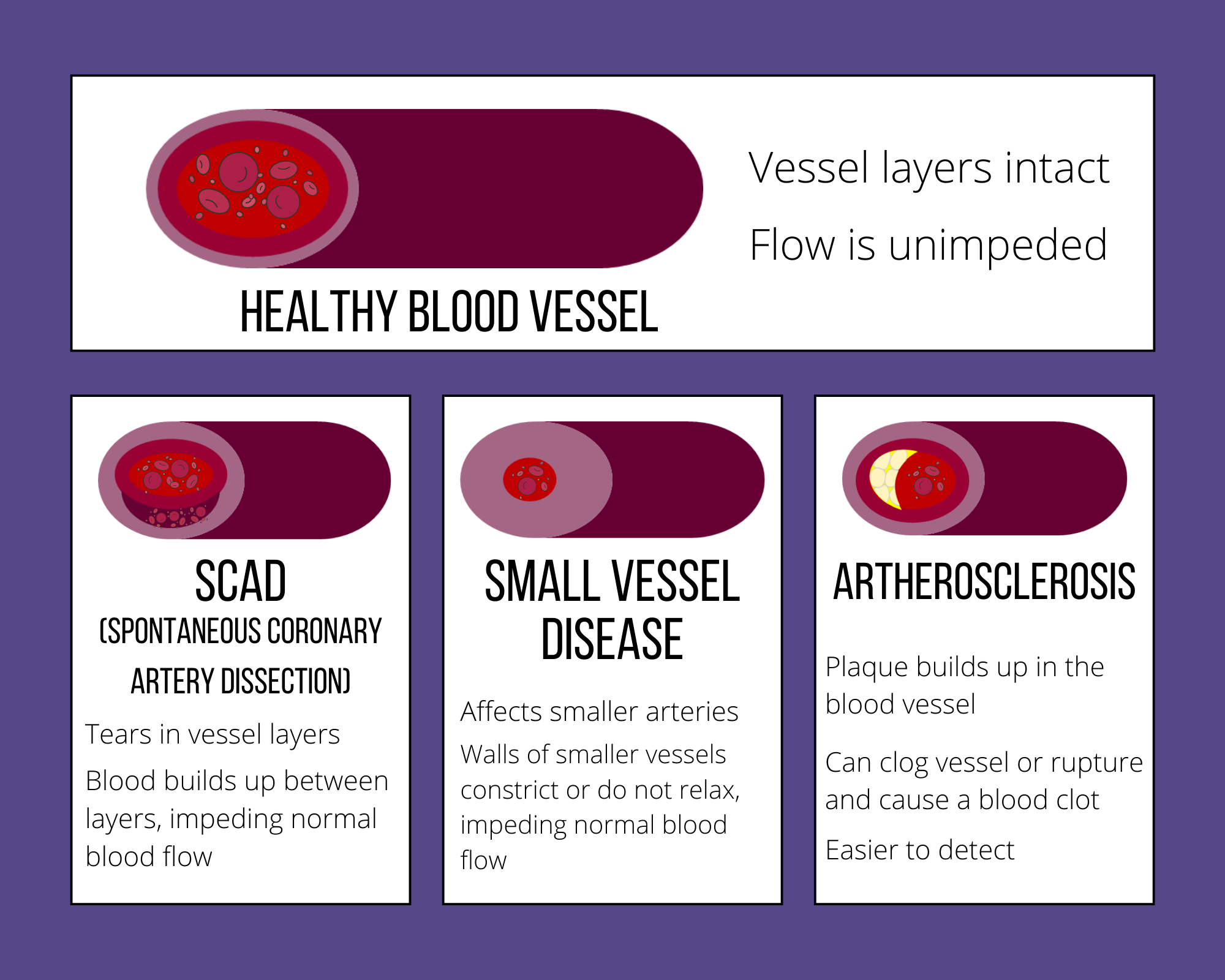
“The clinic at the Women’s Heart Centre focuses on the unique aspects of women’s care. Instead of blockages in the arteries of the heart, women often have small vessel disease or tears in their arteries. They can also have arteries that spasm, which is surprisingly more frequent than previously thought,” says Dr. Sedlak, who is also a cardiologist at St. Paul’s Hospital, Vancouver General Hospital, and British Columbia Women’s Hospital. “To be able to detect these, unique testing is required, so we order specialized MRI imaging and angiograms to focus on looking at small blood vessels.”
Putting this into perspective, a normal cardiac MRI takes about 20–40 minutes; however, Denise was in an MRI machine actively gathering images of her heart for two and half hours. That length of time was needed to confirm that the small vessels in her heart were constricted and preventing blood from nourishing her heart, which explained her symptoms and stress test readings
Research to inform and change practice
Part of the reason for this gender difference in care is because there are fewer clinical studies focusing on women’s heart health specifically. Heart conditions and diseases that were historically thought to be uncommon in women are now increasingly being found. For example, spontaneous coronary artery dissection (SCAD) [illustrated below] was initially thought to be quite rare; however, 90 percent of patients with SCAD are women, so in studies with a predominantly male cohort, it would appear quite rare. This resulted in severe underdiagnosis of an emergent condition that can cause heart attacks.
Dr. Sedlak and her team at the Women’s Heart Centre are working to improve women’s cardiac care. “We have set up a Women’s Heart Centre database. Every woman who comes into the clinic can sign up to be part of the registry, which stores data to support women’s heart research. We have over 300 patients registered who we aim to follow over five years in an effort to better understand the unique aspects of heart health in women. This information will also support research projects to improve heart health overall.”
But what about those who lack access to women’s health-focused clinics or specialized cardiac imaging? Standardizing practice to improve the recognition of heart attacks in women must be addressed as well. That is precisely the research that Dr. Humphries is leading in the Canada-wide multi-center trial, CODE-MI.
“One of the most common ways to detect if a patient has had a heart attack is to look at the levels of a molecule called high-sensitivity cardiac muscle troponin. This molecule is released from the heart as a result of cardiac damage, for example, during a heart attack,” informs Dr. Humphries. “In clinical practice, physicians look at the levels of this molecule in the blood and use a threshold value to help determine whether or not a patient has had a heart attack. Previous research came up with this value based on pooled data from men and women; however, when a woman has a heart attack, less of this troponin molecule is released. Unsurprisingly, the current pooled threshold is higher than the female-specific threshold, increasing the risk that women are underdiagnosed because their levels of troponin after a heart attack do not reach the higher pooled threshold. The goal of the CODE-MI trial is to establish the impact of using threshold values specifically for women to improve the likelihood of an accurate heart attack diagnosis, which will lead to life-saving treatment and care.”
Advocating for change
Denise is far from alone when it comes to overcoming the hurdles to receiving proper care for her heart health. Underdiagnosis of heart disease in women is an international issue that needs to be addressed. Designing clinical trials that actively consider the differences between men and women is important in improving treatment for everyone.
“The more we break down the barriers, the better chance we have of improving care for women,” encourages Dr. Humphries.

In Canada, the wheels of change are starting to turn. Certain funding agencies will not consider supporting research unless there is a clear statement addressing sex and gender, with some even having a minimum threshold for the number of women enrolled. In addition, data supporting the need for a different cascade-of-care plan for women versus men with heart disease are becoming more available, but more work is needed.
System-wide education plays a large role in sparking change and an organization dedicated to spreading awareness is the Canadian Women’s Heart Health Alliance. In 2019, the Alliance initiated the annual country-wide Wear Red Canada campaign on February 13, focused on raising awareness of women’s heart health while providing informative, helpful resources. The Alliance has also developed educational material to be included in high school and medical school curricula, and aims to help inform and improve clinical practice.
Heart to heart
“When in doubt, check it out!” Denise emphasizes. “If something doesn’t feel right, look into it. Advocate for yourself and pay attention to your body because you work in partnership with it. Now, with guidance from my family doctor, the expertise of Dr. Sedlak, and peer support from other women living with heart disease, I have been happily managing my heart health with medication and lifestyle changes for several years.”
Interested in learning more?
The Canadian Women’s Heart Health Centre has several resources available including peer support groups, advice on how to talk to your health care provider, and clinic locations across Canada. They also provide all the resources shared during their Wear Red Canada campaigns, including advice on finding a family doctor.
In addition, the Heart and Stroke Foundation has useful information for anyone curious about heart health and the Canadian Cardiovascular Society provides up-to-date guidelines and resources for health care providers.



