The Evidence Speaks Series is a recurring feature highlighting the latest in CHÉOS research. This series features summaries of select publications and is designed to keep media and the research community up to date with CHÉOS’ current research results in the health outcomes field.
To ensure this research is quick and easy to share, we are now providing social cards that you are free to save and use as you see fit.
More is needed to improve access to emergency contraception in B.C.
Chan MC, Munro S, Schummers L, Albert A, Mackenzie F, Soon JA, Ragsdale P, Fitzsimmons B, Renner R. Dispensing and practice use patterns, facilitators and barriers for uptake of ulipristal acetate emergency contraception in British Columbia: a mixed-methods study. CMAJ Open. 2021;9(4):E1097-104.
In 2015, ulipristal acetate became available as a prescription-only emergency contraceptive in B.C., joining the existing over-the-counter product levonorgestrel. CHÉOS Scientist Dr. Sarah Munro and a team from UBC and the Women’s Health Research Institute set out to understand how ulipristal acetate has been used so far, and the facilitators and barriers for doctors, pharmacists, and patients. Between 2015 and 2018, 318 patients filled 368 prescriptions for ulipristal acetate. While use of the drug increased in this time, significantly more people used levonorgestrel. Speaking with 12 patients, 12 pharmacists, and 15 prescribers, the researchers discovered that use of ulipristal acetate was impeded by lack of awareness and knowledge, concerns about shame and stigma, and health system barriers, such as prescription status and cost. The results highlight the need for more education, training, and advocacy to improve access to emergency contraception in B.C.

—
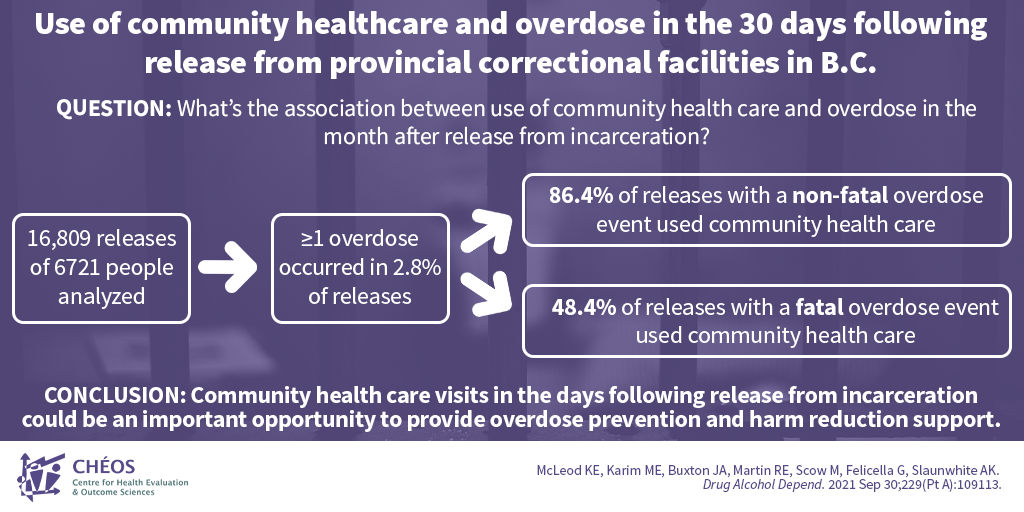
Community health visits may be useful in reducing the risk of overdose after incarceration
McLeod KE, Karim ME, Buxton JA, Martin RE, Scow M, Felicella G, Slaunwhite AK. Use of community healthcare and overdose in the 30 days following release from provincial correctional facilities in British Columbia. Drug Alcohol Depend. 2021;229(a):109113.
In the weeks following release from incarceration, people are at an increased risk of overdose. CHÉOS Scientist Dr. Ehsan Karim worked with researchers from UBC’s School of Population and Public Health and the BCCDC to look into the association between accessing community health care services following release from incarceration and overdose. Of the 16,809 releases analyzed, almost 3% three per cent experienced at least one overdose. While the majority of people who had a non-fatal overdose used community health care before the event (86.4 per cent), less than half of people who had a fatal overdose did the same (48.4 per cent). The results show that community health care visits may be a good opportunity to provide people who have recently been released from incarceration with harm reduction and overdose prevention support.
—
Study highlights factors that may increase the risk of hospitalization among people with COVID
García HAV, Wilton J, Smolina K, Chong M, Rasali D, Otterstatter M, Rose C, Prystajecky N, David S, Galanis E, McKee G, Krajden M, Janjua NZ. Mental Health and Substance Use Associated with Hospitalization among People with COVID-19: A Population-Based Cohort Study. Viruses. 2021;13(11):2196.
CHÉOS Scientists Drs. Caren Rose and Naveed Janjua joined colleagues from the BCCDC to investigate the factors associated with hospital admission among people with COVID-19 in B.C. They included 56,874 COVID-19 cases in the analysis, of which 2,298 were hospitalized. The risk of COVID-19-related hospitalization increased with a number of factors including older age, male sex, pregnancy, chronic comorbidities (e.g., diabetes, chronic kidney disease), substance use, and intellectual and developmental disabilities. These findings have already informed COVID-19 vaccine rollout processes in B.C. and could go on to help health care providers monitor patients who are more likely to experience serious outcomes.