July 28 marks World Hepatitis Day. This year’s theme is ‘Find the Missing Millions’, raising awareness of the 290 million people worldwide who are living with undiagnosed hepatitis.
Closer to home, there is a plethora of ongoing research into hepatitis testing, epidemiology, treatment, and outcomes, including the BC Hepatitis Testers Cohort (BC-HTC).

We spoke with Dr. Naveed Janjua, who leads the BC-HTC, to find out more about how this study is informing hepatitis C elimination efforts in BC and Canada. Dr. Janjua is a CHÉOS Scientist, CTN Investigator, BCCDC Senior Scientist/Executive Director of Data and Analytic Services, and UBC School of Population and Public Health Clinical Associate Professor.
Hepatitis C is a type of liver disease that is caused by the hepatitis C virus. Many people who are infected with the virus show no symptoms and are unaware that they have the disease; however, others may experience a brief illness 6-12 weeks after infection. Diagnosis of hepatitis C involves two blood tests – one to see if you have been exposed to the virus and another to see if the virus is still present in your body. Undiagnosed hepatitis C could lead to a chronic infection, which can be associated with a range of liver disease, from inflammation to life-threatening cirrhosis.
Established in 2013 as a collaboration between the BCCDC, Ministry of Health, and BC Cancer Agency, the BC-HTC includes all individuals who have been tested for hepatitis C or HIV, or been diagnosed with hepatitis B, hepatitis C, HIV or active tuberculosis in BC since 1990. These data are linked with the BC Ministry of Health Client Roster, medical visits, hospitalizations, prescription drug data, cancer registry and mortality, and undergo annual updates.
“The BC-HTC is a large cohort study of 1.7 million people who have been tested for hepatitis C; this represents around a third of BC’s population,” explained Dr. Janjua. “The ultimate goal is to generate knowledge on the epidemiology of hepatitis C, treatment uptake and effectiveness, impact on long-term outcomes, and program progress, in order to inform policy and programming across the nation.”
As discussed in a 2016 paper published by EBioMedicine, monitoring a cohort across different stages of a cascade of care – from diagnosis through to treatment and cure – at a population level allows the measurement of the effectiveness of health care programs and identifies any gaps. Monitoring progress in this way can also help policymakers forecast the economic impacts of different treatments. The BC-HTC ‘provides a population-based benchmark for monitoring the progress of hepatitis care programming to guide policy in British Columbia which can also be used as a framework for other jurisdictions internationally.’
“The BC-HTC acts as a surveillance system,” said Dr. Janjua. “The data we have gathered, and continue to gather, is helping to support efforts to eliminate hepatitis C within the province.”
For example, in research published last year in Liver International, the BC-HTC team analyzed six hepatitis C care cascade stages: antibody diagnosed, RNA tested, RNA positive, genotyped, initiated treatment, and sustained virologic response. They determined that the largest gap in the care cascade was treatment initiation, highlighting that more is needed to ensure that hepatitis C testing and treatment is equitably accessible across the province.
To date, the cohort has produced influential pieces of evidence that have shaped guidelines and policy in Canada and beyond. Further details are available at the website.
—
Dr. Janjua is also Principal Investigator for Hepatitis Education Canada and Co-Investigator for CanHepC; two collaborative projects in Canada that support the elimination of hepatitis C in the country. Together, they developed a blueprint to inform these efforts. (below).
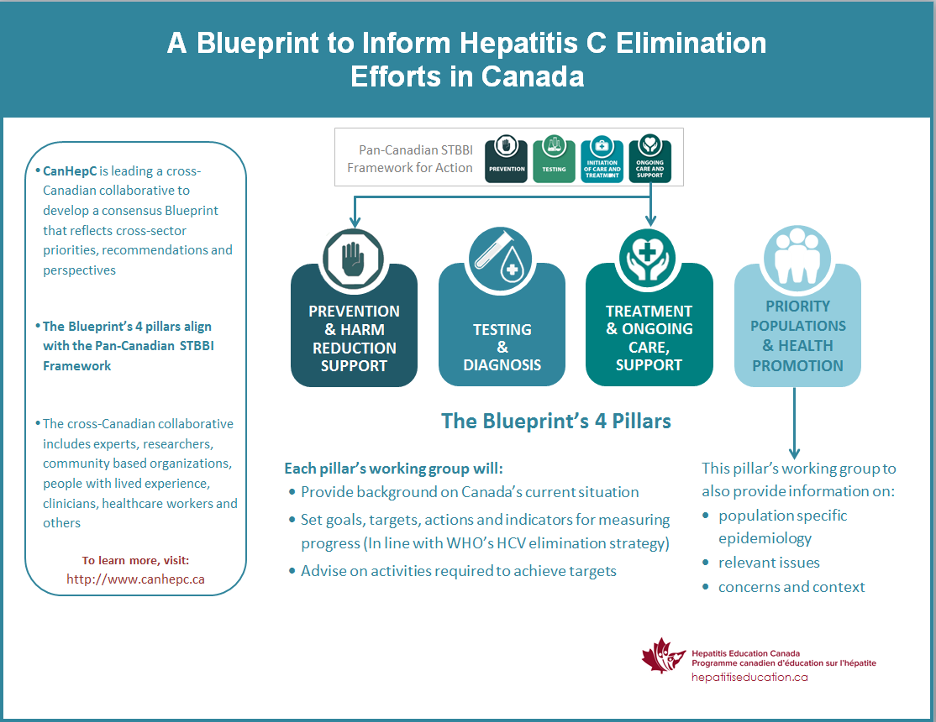
For more information on the projects discussed in this article, please follow the links below:
BC Hepatitis Testers Cohort
Hepatitis Education Canada
CanHepC



