
The first peer-reviewed study in North America examining dosing intervals for COVID-19 mRNA vaccines shows a delayed second dose leads to a stronger immune response. CHÉOS Scientist and principal investigator Dr. Brian Grunau says these results, published today in Clinical Infectious Diseases, could inform ongoing international COVID-19 vaccination efforts.
The team compared blood test results from paramedics who were vaccinated within the currently recommended interval of less than four weeks, to those who received their second dose after six to seven weeks. Participants are enrolled in the larger CORSIP project, a national study examining how the pandemic has impacted paramedics. (CORSIP is still recruiting paramedic participants in British Columbia, Alberta, Saskatchewan, Manitoba, or Ontario.)
“We found significantly higher measures of immunity in individuals who had longer vaccine intervals. This was consistent regardless of which mRNA vaccine was administered,” says Dr. Grunau, who is also an emergency physician at St. Paul’s Hospital and an Assistant Professor at UBC’s Department of Emergency Medicine.

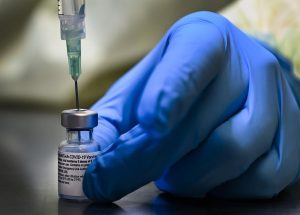
mRNA vaccines include the Pfizer-BioNTech Comirnaty vaccine and the Moderna Spikevax vaccine.
There are limitations to the findings. Although immune measures have been correlated with the risk of contracting COVID-19, the team did not measure actual break-through infections, which is needed to test vaccine effectiveness, explains Dr. Grunau. “To do that, you need a larger sample size. However, you may miss asymptomatic infections. Ideally, our findings could be tested in a clinical trial examining the effect of dosing intervals on break-through infections,” he adds.
Impacting public health decisions in real time
Fast results are crucial right now, as over half of the world’s population has yet to be vaccinated. These findings have implications for the ongoing global vaccination effort. Widening the recommended vaccine dosing interval could potentially lead to a stronger long-term immune response in individuals. It will also facilitate faster community-level access to the first vaccine dose. But choosing which strategy to follow has tradeoffs.
“It may be more advantageous to have doses closer together when there is an extremely high COVID-19 prevalence in the community, or in very high-risk populations such as long-term care residents and immune-compromised individuals,” Dr. Grunau remarks. “However, if your overall goal is long-term protection, then extended intervals may be the preferred strategy.”
As policy-makers in Canada and other jurisdictions lay out groundwork for third doses, this study adds to the growing evidence that a longer interval between doses produces a better and prolonged immune response. This could potentially play a role in the timing and need for a third dose.
“It is possible that individuals with a longer interval between their first two doses may not require a third shot as early,” Dr. Grunau comments.
How COVID-19 has changed the speed of research
The larger CORSIP project is funded by the federal government’s COVID-19 Immunity Task Force (CITF). The team is co-led by Dr. David Goldfarb, a clinical associate professor in the Department of Pathology and Laboratory Medicine at UBC and a medical microbiologist and infectious disease specialist at BC Children’s Hospital, as well as Drs. Tracy Kirkham and Paul Demers from the University of Toronto. They started recruiting paramedics less than 10 months ago, but, like many other ongoing COVID-19 studies, researchers are feeding data in real-time to the CITF so decision-makers can determine if there are implications for policy decisions
As Dr. Grunau shares, usually with research, it takes years to design and implement a project, and then submit results for publication. “Then, we aim to convince clinicians and policy makers to examine our results and hope that practice is eventually impacted. But with COVID-19, things have definitely gone warp speed.”
While this constant stream of new information can make things difficult for those who have to make public health decisions, for researchers, it has been rewarding to see their efforts translate into clinically relevant findings.
As Dr. Grunau sums up, “That is the real goal of any researcher: we want to do research that will actually positively impact people’s lives and affect policy.”



